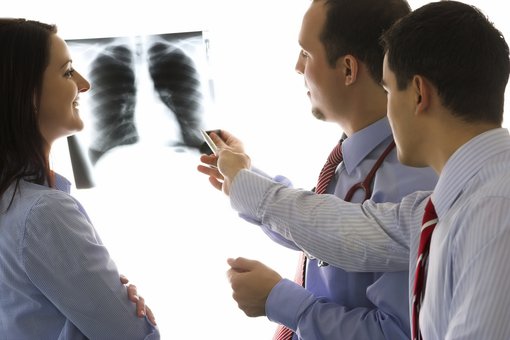
Since the pandemic took hold in Fiji, doctors from across the world have gathered on Zoom once a fortnight to help the country navigate the virus.
"The medical side in Fiji have greatly benefitted from our... COVID-19 discussion forums," Dr Chris Hair FRACP told Pacific Beat.
For a decade Dr Chris Hair, a gastroenterologist based in Geelong, has travelled to Fiji to train healthcare workers in endoscopy.
In 2016, Dr Hair started organising online webinars for endoscopic training back in 2016 as a volunteer with the Australian and New Zealand Gastroenterology International Training Association.
But watching COVID-19 cases swell in Fiji prompted Dr Chris Hair to adapt the virtual training program to teach doctors about coronavirus instead.
Fiji National University's Dr Mai Ling Perman believes the program is helping.
"We've had sessions where the doctors from the main hospital in Suva that would present a case that might be COVID or vaccine related where we discuss and apply," she said.
ABC Online, 6 September 2021
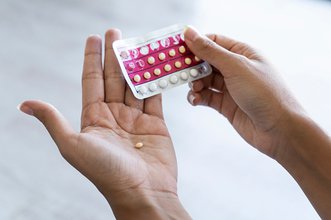
Blood clots have been getting a lot of media attention.
You may even have heard the statistic that you're more likely to get a blood clot from the contraceptive pill than a COVID-19 vaccine. But thankfully, that doesn't mean blood clots are common among people taking the pill. They're actually very rare.
We asked two experts exactly what that risk is; what individual factors can increase that risk; and what your best contraceptive options are if you are in a higher risk category.
Do you need to be worried?
"The short answer is no. you don't have to be concerned," says Dr Tonia Mezzini FAChSHM, a sexual health physician based in Adelaide.
About five to seven out of every 10,000 women taking the "bog standard," older, combined oral contraceptive pill will get a blood clot, she says. That's about 0.05 per cent of these pill-takers — only a small increase on the number of women not taking the pill at all (of which about two in every 10,000, or 0.02 per cent, will get a clot in their leg or lungs).
The risk of developing a clot goes up slightly if you're using a newer pill with drospirenone, "which is in [a product] like Yas or Yasmine," Dr Mezzini says.
If you're using one of those pills, then the risk increases to about 9 to 12 out of 10,000 women.
"So it's a very low chance of having a clot, but it does increase depending on the type of pill you use," she says.
ABC Online, 25 August 2021
Heart complications in Australians who caught severe COVID-19 during 2020 were less common than feared, although early overseas evidence suggests the Delta variant could have a greater impact on cardiovascular health.
Initial results from the ongoing AUS-COVID trial, led by Sydney’s Royal North Shore Hospital, and published in the Medical Journal of Australia, found fewer than one in 25 hospitalised COVID-19 cases developed an atrial fibrillation, or heart flutter. The rate was higher – one in 16 – for patients aged 65 and over.
Researchers analysed the medical records of 644 consecutive COVID-19 patients admitted to hospital in 2020.
Professor Ravinay Bhindi FRACP, head of cardiology at Royal North Shore Hospital, said the study began in May 2020 amid early data from China, Europe and the US that suggested patients who had heart disease fared worse when exposed to COVID-19.
The study, which has an average patient age of 62, was then expanded to involve patients who did not have a history of heart disease.
While the study showed rates of death in hospitalised COVID-19 patients consistent with overseas data, Professor Ravinay said Australia’s rate of cardiac disease and events was “much less”.
“In terms of serious complications, they did only occur in a very small proportion of patients,” he said.
The study’s authors said the results were “reassuringly low”, although they said they did not have information on the patients after their discharge from hospital and some heart complications such as heart failure and myopericarditis may take weeks to become apparent.
“While clinicians should remain vigilant, the incidence of clinical cardiac complications during index hospitalisations was reassuringly low,” they said.
The Sydney Morning Herald, 6 September 2021
South Australia has now become the fourth state to legalise voluntary euthanasia.
The Voluntary Assisted Dying Bill passed the House of Assembly on Thursday morning.
The laws are expected to come into effect in 18 months – but how will it work?
The Advertiser spoke with Melbourne-based VAD-trained oncologist Dr Phillip Parente FRACP. The Monash University Associate Professor has been providing VAD assessment since March 2020.
Several of the specialist’s oncologist patients were among 224 Victorians who have died using VAD in the law’s first 18 months.
Dr Parente, who once opposed VAD based on his Catholic beliefs, said all of his patients to date had self-administered the VAD medication after a thorough and rigorous application process that takes no fewer than nine days, and on average 19 days, to complete
“They must have capacity to administer the medication on their own, unassisted,” he said. Patients unable to swallow or too weak to self-administer can apply for intravenous practitioner administration.
The Advertiser, 24 June 2021
Dr Elisabetta Puglisi FRACP has taken on an expanded role at Portland District Health as part of the health service’s growing status as a training organisation.
As the Director of Clinical Training, Dr Puglisi, who has been with PDH since last July as a general physician, is ensuring the expanded training programs are meeting their targets.
PDH’s director of medical services Dr Kaushik Banerjea said the role was needed to supervise the various training programs.
“We are now a training organisation of significance and as we’ve become more involved in the training of doctors, there was a need for a director of clinical training to oversee these programs,” Dr Banerjea said.
Portland Observer, 3 August 2021


Australia’s low death rate from the rare syndrome linked to the AstraZeneca shot is in no small part due to a ‘huge collaborative effort’.
It was during an urgent meeting to discuss a baffling blood-clotting condition that haematologist Professor Huyen Tran FRACP received the call he knew was inevitable.
“The adrenaline began to run a bit,” Tran, the director of the Ronald Sawers Haemophilia Centre in Melbourne, says.
“But the one thing that I’ve learned over the years is when you see a very difficult situation, you don’t panic. You take a step back and you calmly think through the problem and present the solution.”
The call, on 1 April, was about a 44-year-old health worker, who had just turned up to a Melbourne emergency department complaining of fever, fatigue, head fogginess, and serious abdominal pain. Eight days earlier, he had received his first dose of the AstraZeneca Covid-19 vaccine.
A medical worker prepares to give a patient a shot of the AstraZeneca coronavirus vaccine.
The rollout of the AstraZeneca vaccine had begun in Australia just a couple of weeks before the meeting.
At the time a condition known as TTS, also called vaccine-induced thrombotic thrombocytopenia, was being described by countries where the vaccine had been administered for months. It was being triggered by an extreme immune system reaction. The condition led to a low platelet count, and often to blood clotting in arteries and veins at unusual sites in the brain and abdomen. Mortality was high; between 25% and 50% of those with TTS died in those first months.
That first Melbourne patient, though severely affected by TTS clotting in the abdomen and requiring surgery, survived.
“That first case was so important as it taught us a lot,” Tran says.
The Guardian, 2 October 2021
Members in the media
Members in the media
‘Reassuringly low’ rates of heart problems in first wave COVID-19 patients
‘Reassuringly low’ rates of heart problems in first wave COVID-19 patients
‘Just in time’: how Australian doctors drastically reduced deaths from vaccine-linked blood clots
‘Just in time’: how Australian doctors drastically reduced deaths from vaccine-linked blood clots
Keeping kids well the focus
of new national mental
health strategy
Keeping kids well the focus
of new national mental
health strategy